Podcast: Play in new window | Download
For some people, rhodium’s most important aspect is its high price. For others, it’s absolutely priceless.
Featured above: Many people keep their rhodium close to the vest.
Show Notes
A Note On Notes: I hope you’ll forgive a week of rather meager show notes! Traveling over Labor Day really took a big bite out of my production process, and I wound up scrambling to complete today’s episode. The show notes, sadly, are the first victim of poor time management.
By Any Other Name: Some of rhodium’s salts are a rich rosy color, and rhodon is Greek for “rose.” That’s all there is to it! I didn’t think it was quite interesting enough to include in the episode.
Interestingly, Rhode Island is a quite controversial name — both halves! It’s not an island, and the origins of “Rhode” are somewhat murky.
Coming Up: I’m back on track for palladium, and I miiiight have a few other neat things in the pipeline. I’ll post about them here on the blog if they come to pass. Stay tuned!
Episode Script
Like the refractory metals, and other sub-categories on the periodic table, “precious metals” are somewhat loosely defined. There are a couple no-brainers in the group — gold, silver, platinum — but plenty of others could be included, depending on who you ask. Palladium and iridium are often counted as precious metals, and sometimes, even metalloids like germanium earn this designation.1
The reason it’s so loosey-goosey is because the definition of a precious metal is determined mostly by its market price rather than anything to do with chemistry or metallurgy.
While those other metals enjoy greater recognition, it’s actually rhodium that usually tops the price charts. Element 45 tends to cost more than triple the price of gold, silver, or platinum by weight.2 It’s not very difficult to make the case that, by the only metric that counts, rhodium is the most precious metal of all.3
But there are millions of people for whom rhodium is worth even more — regardless of the commodities market. You simply can’t put a price tag on something that keeps you alive.4
You’re listening to The Episodic Table Of Elements, and I’m T. R. Appleton. Each episode, we take a look at the fascinating true stories behind one element on the periodic table.
Today, we got the beat with rhodium.
In general, rhodium is very similar to its platinum-group neighbors. William Hyde Wollaston discovered element 45 in 1803, soon after he discovered element 46, palladium. It’s often employed as a catalyst in chemical reactions, and sometimes as an ornamental metal. And Geoffrey Wilkinson was a big fan. He’s the platinum-group enthusiast who called ruthenium “an element for the connoisseur,” and he was no less thrilled for rhodium.
Wilkinson spent most of his career at the Imperial College in London, and uncovered a lot of advanced knowledge about today’s metal.5 One day in 1961, he locked himself in his laboratory alone — a circumstance that the Platinum Metals Review notes was “something that always terrified his students.”6 When he finally burst forth from confinement, he held aloft a test tube full of a new rhodium compound, a bubbling, brown, boiling-hot liquid, and triumphantly hollered, “Who wants a Ph.D.?”7
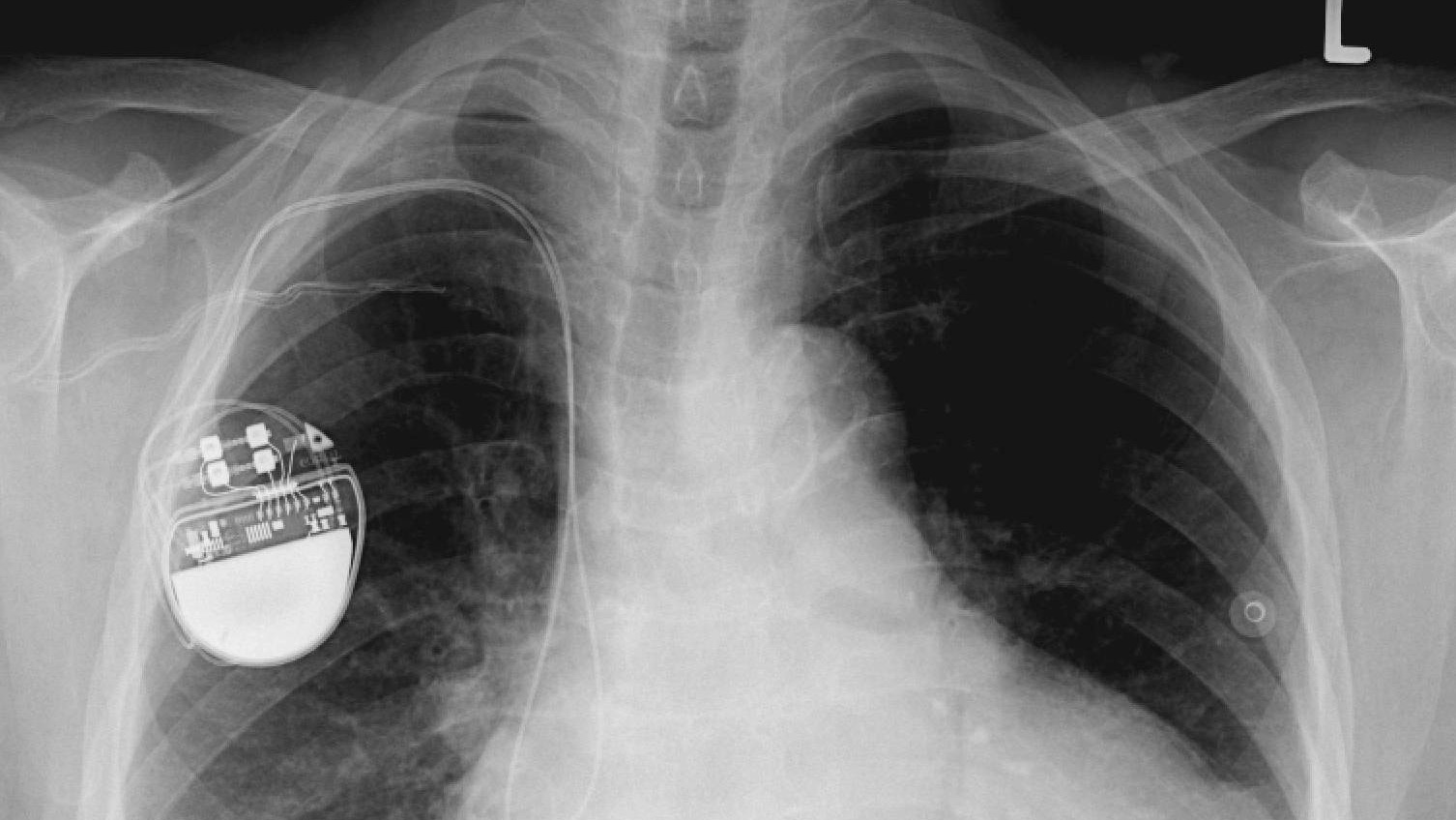
You’d be hard-pressed to find anyone else whose heart could race so quickly for rhodium. In a way, that’s by design: rhodium is an important component in that cardiac regulator known as the pacemaker.
We get to pick up this story where a prior episode left off. With zinc, we learned about the myriad and sundry grotesque ways that Romantic-era Europeans amused themselves with powerful electrical currents and corpses in various stages of repose.
Despite their best efforts, the brightest minds of the day eventually learned that electricity cannot resurrect the dead. But it can be a different story for someone who’s only mostly dead. Like Miracle Max said, “there’s a big difference between mostly dead and all dead. Mostly dead is slightly alive.”
Sometimes it’s possible to bring a person back from the brink by applying just the right amount of electricity to just the right spot. We’ve been working on that technique since the 1700s, although our earliest attempts were slightly less sophisticated than what we do nowadays.
Englishman Charles Kite described one early case in 1788. A three-year-old girl had fallen out of a high window and was presumed dead after an apothecary’s attempts to revive her were unsuccessful. Having little left to lose, the apothecary administered electrical shocks more or less randomly around her body.
Twenty minutes had at least elapsed before he could apply the shock, which he gave to various parts of the body without any apparent success; but at length, on transmitting a few shocks through the thorax, he perceived a small pulsation; soon after the child began to sigh, and to breathe, though with great difficulty. In about 10 minutes she vomited. A kind of stupor remained for some days, but the child was restored to perfect health and spirits in about a week.”8 9
That’s a truly astounding feat, especially since twenty minutes without oxygen would typically result in heavy brain damage. But similar reports of electrical resuscitation started to spring up elsewhere in Europe around the same time.10
That’s not really a pacemaker, though. It’s more akin to a defibrillator, which, incidentally, might not do what you think it does.
On television, doctors will reach for the paddles when a patient’s heart stops beating. They’ll administer a shock, and with luck, the patient’s heart will start to beat again.
This is the opposite of how a defibrillator really works. In real life, the device is used to treat patients whose hearts are still beating, but with a pattern that’s too fast, too slow, or simply erratic. When doctors deliver the shock, they’re actually stopping the heart. Ideally, the body then notices that the heart has stopped pumping, and will start again clean, with a regular beat that’s neither too fast nor too slow.11 12
It’s kind of like when your computer starts popping up error messages faster than you can read them, so you just smash the restart button. A defibrillator doesn’t power up a heart that’s stopped, it reboots a heart that’s acting wonky.
It wasn’t until 1926 that we targeted the “sinoatrial node,” a small region of the heart that naturally governs the heartbeat. Dr. Mark Lidwill was attempting to revive a stillborn infant after all other methods had failed. Applying an electrified needle to this precise spot of the child’s heart and delivering regular, consistent shocks allowed Lidwill to operate the heart in a sort of “manual override” mode. As he described, “At the end of ten minutes the current was stopped and it was found that the heart would beat of its own accord. The child recovered and is now living, and quite healthy.”13
Lidwill is one of many people to get credit for inventing the pacemaker, a claim that’s kind of true and kind of not. We can’t really point to the one person who invented the pacemaker, because in fact, dozens of people are responsible for the slow discovery and improvement of the technology. It’s like how Mendeleev didn’t come up with the idea for the periodic table single-handedly, but built on the work of those who came before, and his work was improved by those who came after. History isn’t so much a blade forged by individual smiths as it is a stone that’s slowly shaped by all of us as it tumbles through time.
However, we can point to the one person who gave the device its name. That would be Albert Hyman, working only a few years later. The biggest problem with Lidwill’s version was that it had to be plugged into a “lightning point,” that is, a wall socket. It was only useful so long as the patient was plugged in, so to speak, and carried a rather high risk of lethal shock.
Hyman created and patented the first invention on the books to be called a “pacemaker,” and it’s his term that we use today. It was portable — technically. It was about the size of a desk, weighed several pounds, and was powered by a hand-cranked spring motor. This version of the pacemaker must have been rather intimidating. Critics decried it as “an infernal machine that interfered with the will of God,” and Hyman never found anyone willing to mass produce the thing.14 15 16
It’s too bad, because Hyman’s invention worked well, and he possessed a sophisticated understanding of why it worked, unlike his predecessors. He probably deserved greater success — but at least he contributed to the body of knowledge.17
Many others made incremental improvements. The engineer Jack Hopps came up with a way to insert an electrified catheter through a vein, a much less intrusive way to administer aid. Coincidentally, several decades later, his own life was saved by an artificial pacemaker.18 19The Canadian Medical Journal ran an article with the headline, “Canadian Engineer Left To His Own Devices.”20
It’s that kind of pacemaker that benefits from the use of rhodium. It conducts electricity better than any other platinum-group metal, but it has the same resistance to corrosion as its siblings. It’s also a material that the body tolerates well.21
That’s especially important for those pacemakers that came next, which were instruments that could actually be implanted in a patient’s body, to provide constant, long-term care.
The first person to receive such a treatment was Arne Larsson, and depending on your perspective, he was a man who was either extremely unlucky or incredibly fortunate.
In 1956, Larsson ate some tainted oysters, which left him with more than an upset stomach. The spoiled shellfish actually gave him hepatitis, and that escalated into a problem called Stokes-Adams syndrome. The condition caused his blood pressure to occasionally drop precipitously, leading to fainting spells that could potentially be lethal.22 Some days, he needed to be resuscitated twenty or thirty different times by medical aides or his wife, Else-Marie, pounding his chest.23
At the time, Drs. Ake Senning and Rune Elmqvist were trying to design an implantable pacemaker, but it was still a prototype. It wasn’t ready for human trials. But Arne and Else-Marie were desperate for help.24
Despite his reservations, Senning agreed to conduct the surgery. On October 8, 1958, the 43-year-old Arne Larsson became the first person to receive an implanted pacemaker. It was the shape and size of a very thin hockey puck.25
A few hours later, on October 8, 1958, the 43-year-old Arne Larsson became the first person whose implanted pacemaker failed.
Luckily, Elmqvist had built a backup just in case this kind of thing happened, so on October 8, 1958, the 43-year-old Arne Larsson became the first person to receive a second implanted pacemaker.
That actually became kind of a regular procedure for him. Over the next four decades, Larsson underwent twenty-five separate operations to replace his artificial pacemakers.26 But make no mistake: Despite needing regular tune-ups, he enjoyed a full and healthy life traveling the world. He actually outlived both Dr. Elmqvist and Dr. Senning. Larsson lived to be 86 years old, dying from complications of melanoma in 2001.
Nowadays, artificial pacemakers are much smaller and considerably more sophisticated, and the risk associated with their implantation is much lower.27
Nonetheless, you don’t need to undergo general anesthesia just to acquire element 45. Rhodium is extremely expensive, but it only takes a very small amount to plate jewelry in a thin coating of the element. This manages to provide a bright shine that never tarnishes without increasing the cost by a factor of ten.
It performs a less glamorous role as part of those catalytic converters we discussed last episode. Those are also pretty easy to remove from a parked car. It only takes a couple minutes and a reciprocating saw. Sadly, this has become common knowledge among thieves, and the rising price of precious metals has caused an increase in catalytic converter theft.28
If you don’t want to turn to a life of crime, and aren’t willing to go under the knife for unnecessary cardiac surgery, there’s another way to acquire element 45 without forking over gobs of cash: Just become the all-time best-selling recording artist in history. In 1979, that person was Paul McCartney, and the Guinness Book of Records paid tribute by awarding him a record plated with rhodium. More valuable, obviously, than gold or platinum.
Of course, if you do manage to become so renowned, you can probably afford the $5,000-an-ounce prize tag that rhodium commands.29 30 However you get your hands on rhodium, you’ll probably have to work pretty hard for it — an effort that’s sure to keep this element close to your heart.
Thanks for listening to The Episodic Table of Elements. Music is by Kai Engel. To learn what rhodium is named after, visit episodic table dot com slash R h.
Next time, we’ll see how crafty Dr. Wollaston could be when we discover palladium.
Until then, this is T. R. Appleton, reminding you that it is generally inadvisable to subject an unconscious person to a high-powered electrical shock, just to see what happens.
Sources
- Northeast Precious Metals, Germanium.
- InvestmentMine, Precious Metals Investing — Commodity Closing Prices.
- MarketWatch, Pros And Cons Of Investing In Rhodium, A Precious Metal Over Twice As Valuable As Gold. Myra P. Saefong, March 22, 2019.
- Circulation, Cardiac Pacemakers From The Patient’s Perspective. Mark A. Wood and Kenneth A. Ellenbogen, May 7, 2002.
- Biography of Geoffrey Wilkinson from The Royal Society Of London, p. 600 (PDF)
- Platinum Metals Review, Sir Geoffrey Wilkinson: New Commemorative Plaque. (PDF) W. P. Griffith, 2007.
- ibid.
- An Essay On The Recovery Of The Apparently Dead, p. 165-166. Charles Kite, 1788.
- The Annual Register, Or, A View Of The History, Politics, And Literature For The Year 1783, p. 107. J Dodsley, 1783.
- The Textbook Of Emergency Cardiovascular Care And CPR, p. 194. John M. Field, 2009.
- The Debunker, Can Defibrillators “Restart” A Stopped Heart? Ken Jennings, 2016.
- ScienceABC, Defibrillator: What Is A Defibrillator? How Does It Work To Revive Patients? 2018.
- The Evolution Of Cardiac Surgery, p. 183. Harris B. Schumacker, 1992.
- Texas Heart Institute Journal, Brief History Of Cardiac Heart Pacing. Glen D. Nelson, MD, 1993.
- Brought To Life Science Museum, Pacemaker.
- The New York Times, Albert Hyman, 79, Cardiologist, Dies. December 9, 1972.
- Indian Pacing And Electrophysiology Journal, Early History Of Cardiac Pacing And Defibrillation. Seymour Furman, MD, January 1, 2002.
- BC Medical Journal, John Hopps And The Pacemaker: A History And Detailed Overview Of Devices, Indications, And Complications. Perminder Bains, MD et. al., January/February 2017.
- CBC, Meet The Canadian Engineer Who Casually Invented The Pacemaker. Chris Chang-Yen Phillips, February 28, 2017.
- Canadian Engineer Left To His Own Devices. CMAJ, October 1, 1997.
- Materion Brush Performance Alloys Technical Tidbits, The Platinum Group Metals As Coating Materials. (PDF) Mike Gedeon, 2012. If “Materion” rings a bell, it’s because they were the corporate villains from Episode 4, Beryllium. I wouldn’t cite them as a source on how toxic a given material is, but for easily verifiable physical properties, they’re as good a resource as anyone.
- Associated Press, Arne Larsson, 86; Had First Pacemaker. January 16, 2002.
- The New York Times, Arne H. W. Larsson, 86; Had First Internal Pacemaker. Lawrence K. Altman, January 18, 2002.
- Machines In Our Hearts: The Cardiac Pacemaker, The Implantable Defibrillator, And American Health Care, this page. Kirk Jeffrey, April 1, 2003.
- The Edge Of Medicine: The Technology That Will Change Our Lives, p. 134-135. Dr. William Hanson, M.D. 2008.
- The New York Times, The Doctor’s World: After 40 Years, Pacemakers Are Smarter And Safer. Lawrence K. Altman, October 27, 1998.
- Journal Of The American College Of Cardiology, Cardiac Pacemakers: Function, Troubleshooting, And Management: Part 1 Of A 2-Part Series. Siva K. Mulpuru, MD et. al.,January 17, 2017.
- Forbes, Catalytic Converter Thefts Plague Car Owners – Here’s How To Slow Down Thieves. Josh Max, April 2, 2019.
- Kitco, Rhodium Prices Going Higher, Analysts Eyeing $10,000. Neils Christensen, August 28, 2019.
- Infomine, Rhodium Price Chart: One-Year.